From Bruises to Diagnosis: Recognizing and Managing Medication-Induced Hyperpigmentation
Overview
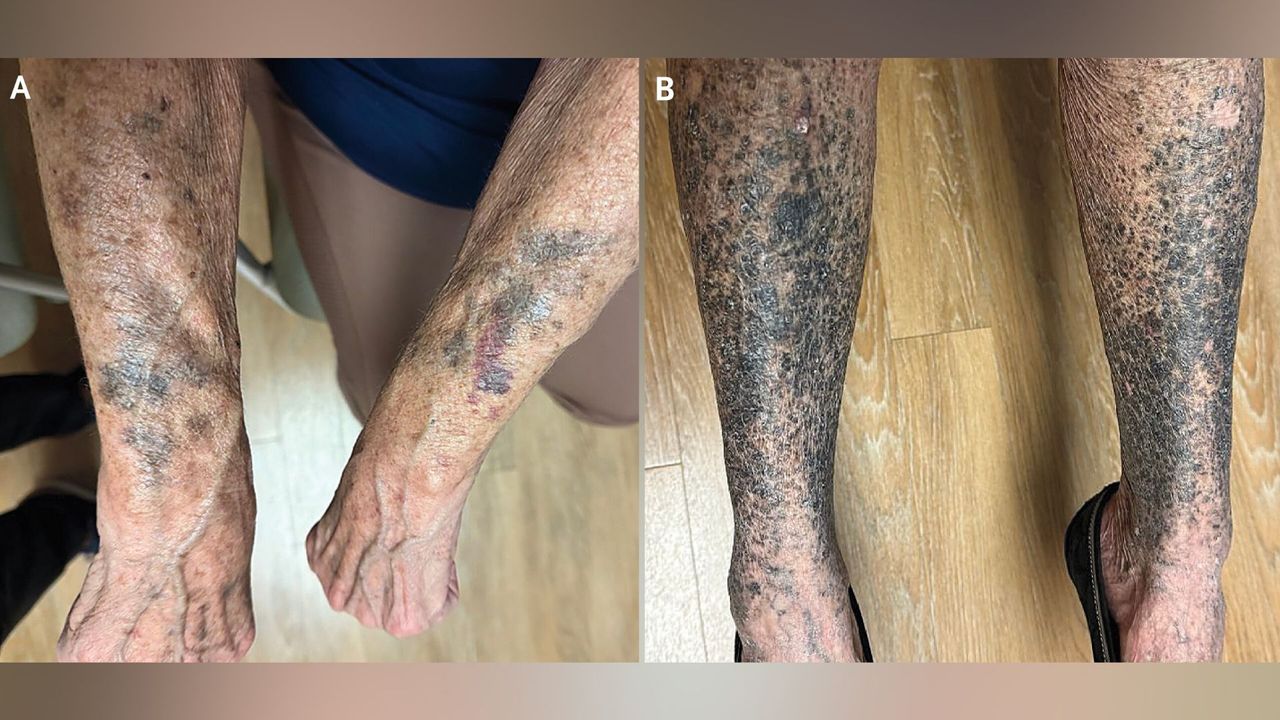
Imagine a patient who, weeks after starting a new prescription, notices her skin turning patchy black and blue—like a fading bruise that never goes away. This isn’t a rare freak accident; it’s a classic presentation of medication-induced hyperpigmentation. While the original case highlights a woman experiencing sudden pigment changes after a new drug, the phenomenon is far broader. This guide will walk you through the recognition, evaluation, and management of drug-related skin darkening, blending clinical pearls with practical steps. Whether you’re a healthcare provider, a pharmacist, or a curious patient, you’ll learn how to connect the dots between medication exposure and skin discoloration, and what to do about it.
Prerequisites
Before diving into the diagnostic process, ensure you have:
- Basic knowledge of common hyperpigmentation causes (e.g., sun damage, melasma, post-inflammatory hyperpigmentation).
- Access to patient’s medication history (including over-the-counter drugs, supplements, and topical agents).
- Familiarity with drug classes known to cause pigmentary changes (see table below).
- A Wood’s lamp or skin biopsy capability (for confirmation in ambiguous cases).
Step-by-Step Diagnostic and Management Guide
Step 1: Recognize the Clinical Pattern
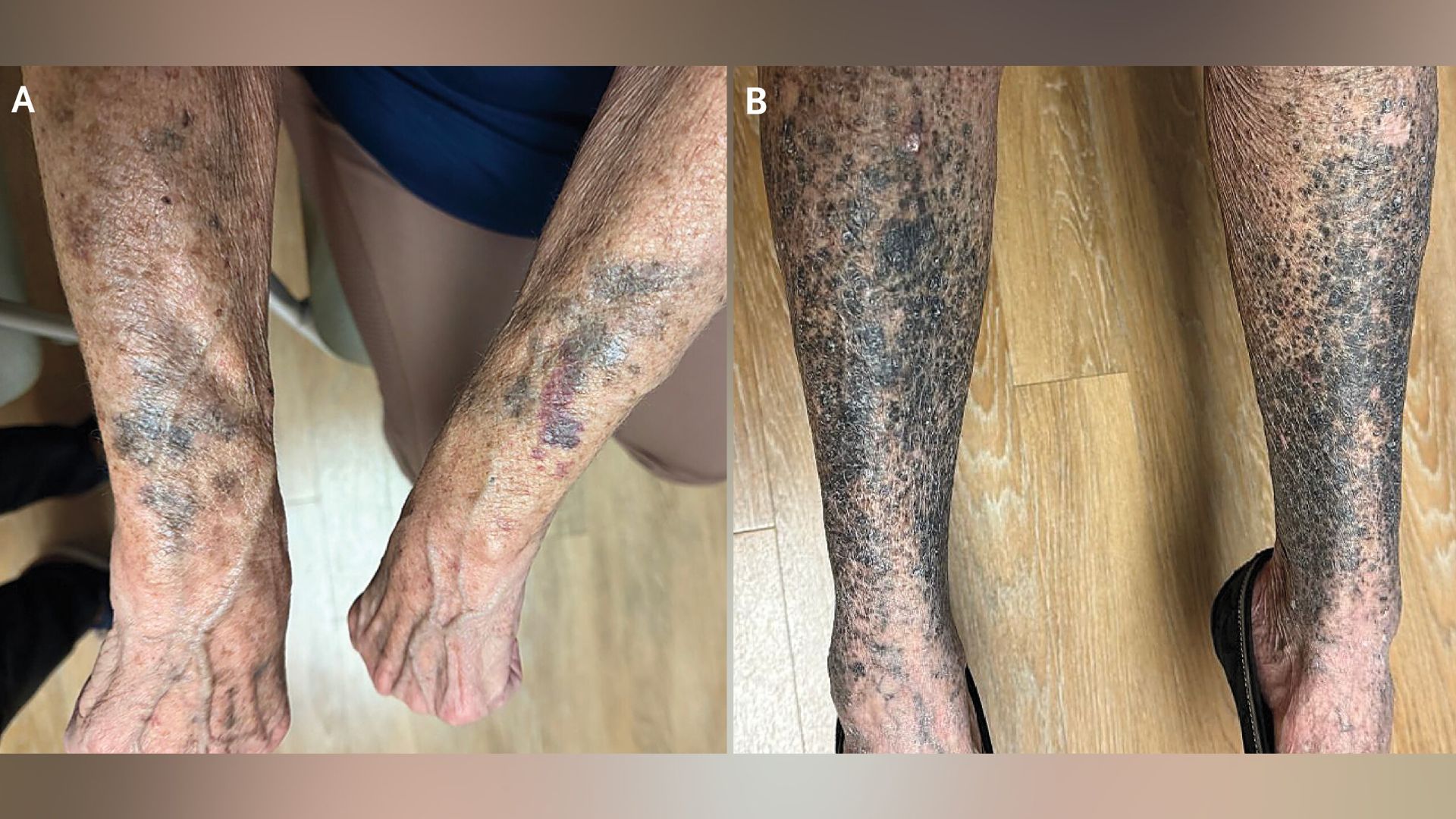
Medication-induced hyperpigmentation often appears as well-defined patches of brown, blue-gray, or black discoloration. Key clues include:
- Timing: Onset days to months after starting a new drug.
- Location: Sun-exposed areas (face, neck, arms) or sites of friction. Some drugs cause diffuse pigmentation.
- Associated symptoms: Usually no itching or scaling, but sometimes photosensitivity.
For example, the woman in the original case likely developed symmetrical, non-pruritic patches on her cheeks and knuckles—a giveaway for drug involvement.
Step 2: Review the Medication List
Common culprits include:
| Drug Class | Examples | Pigment Characteristics |
|---|---|---|
| Antimalarials | Hydroxychloroquine, chloroquine | Blue-black on shins, palate |
| Amiodarone | Antiarrhythmic | Slate-gray on sun-exposed skin |
| Oral contraceptives | Estrogen/progestin | Melasma-like brown patches |
| Chemotherapeutic agents | Bleomycin, busulfan | Linear hyperpigmentation over veins or transverse bands |
| Heavy metals | Gold, silver (argyria) | Blue-gray diffuse |
Step 3: Perform a Focused Physical Exam
Use a Wood’s lamp to differentiate melanin from other pigments. Melanin darkens under UV light; drug deposits (like amiodarone) may not. Note distribution: symmetrical? On scars? Nail involvement?
Step 4: Order Confirmatory Tests (if needed)
- Skin biopsy: Shows pigment incontinence or drug deposits in macrophages.
- Dermoscopy: Reveals brown blotches or steel-blue structures.
- Blood levels: For drugs like amiodarone or minocycline.
Step 5: Discontinue or Switch the Culprit Drug
If possible, stop the offending agent. Reversal may take months to years. For essential drugs (e.g., amiodarone in arrhythmias), consider dose reduction or alternatives.
Step 6: Manage Residual Pigmentation
- Sun protection: Broad-spectrum SPF 50+.
- Topical agents: Hydroquinone, tretinoin, or kojic acid for melanin-based hyperpigmentation.
- Laser therapy: Q-switched Nd:YAG for blue-gray deposits.
- Cosmetic concealment: Camouflage makeup.
Common Mistakes
Mistake 1: Attributing Pigmentation to Sun Exposure Alone
Many doctors assume new spots are just sun damage. Always take a thorough drug history.
Mistake 2: Not Considering Over-the-Counter Products
Herbal supplements, niacinamide, or even some eye drops can cause discoloration.
Mistake 3: Stopping an Essential Medication Without Alternatives
Abruptly ceasing a life-saving drug can be dangerous. Collaborate with the prescribing specialist.
Mistake 4: Biopsying Without Proper Clinical Context
Biopsy may show non-specific melanosis. Always correlate with timing of drug exposure.
Summary
Medication-induced hyperpigmentation is a reversible cause of skin darkening that demands a high index of suspicion. By following this step-by-step guide—recognizing patterns, reviewing medications, using confirmatory tests, and managing effectively—you can turn a diagnostic dilemma into a straightforward solution. Always remember: when the skin turns black and blue weeks after a new drug, the culprit is often hiding in the medicine cabinet.
Related Articles
- 7 Things You Need to Know About the New Attack on AMA's Billing Codes
- How to Navigate FDA Approval for an Alzheimer’s Agitation Therapy
- 5 Lessons from GitHub's Rate Limiting Overreach: When Defenses Become the Problem
- A Step-by-Step Guide to Creating Wheat Hybrids with 70% Resistance to Fusarium Head Blight Using Genetic Loci from Elymus repens
- The Silver Screen's Health Impact: How Media Portrayals Shape Real-World Behaviors
- Hinge’s New FDA-Cleared Migraine Device: A Breakthrough in Non-Invasive Relief
- Bridging the Gap: A Guide to Including People of Color in the Psychedelic Renaissance
- New Single-Cell Imaging Technique Reveals the Dynamics of Stalled DNA Replication